

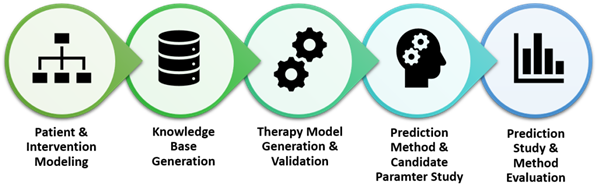

The initial goal is to establish a general understanding of the coiling patterns and their impact on the convalescence of spinal perfusion and the clinical outcome. Initially, an extensible patient model needs to be developed including multi-modal imaging & procedure parameters, e. g. blood pressure, heart rhythm, CVP, rMAP as well as anatomical parameters, such as Crawford classification, calcification status and artery kinking. Following the model generation, an analysis of the MISACE procedures will be conducted investigating the correlation between coiling patterns and patient outcome. For the support of the treatment planning phase, a prediction method to estimate patient-individual consequences of coiling patterns on the overall procedure risk, the minimal recuperation time and ultimately, the clinical outcome will be developed and evaluated. A therapy support system for the MISACE procedure will then be developed to support the pre-operative treatment planning including the prediction of consequences for coiling patterns on the clinical outcome as well as the overall procedure risk.
Patients suffering from large thoracoabdominal aortic aneurysms (TAAA) are often confronted with the need for substantial aortic repair procedures achieved with artificial aortic valve replacement. The risks of such an intervention lies with the acute reduction of tissue vascularization resulting in neurological pathologies, e. g. paraplegia.The minimally invasive, selective segmental artery coil embolization (MISACE) is a procedure employed to preemptively close supplying segmental arteries of the aorta to promote collateral perfusion network arteriogenesis prior to such a conservative procedure. Since the MISACE procedure is still in an early application phase there exist no general guidelines for artery closing patterns and their respective influence on the clinical outcome. Furthermore, the impact on the paraspinal collateral network perfusion compensation mechanics and the corresponding risk of ischemia and paraplegia are unknown.

Um dir ein optimales Erlebnis zu bieten, verwenden wir Technologien wie Cookies, um Geräteinformationen zu speichern und/oder darauf zuzugreifen. Wenn du diesen Technologien zustimmst, können wir Daten wie das Surfverhalten oder eindeutige IDs auf dieser Website verarbeiten. Wenn du deine Zustimmung nicht erteilst oder zurückziehst, können bestimmte Merkmale und Funktionen beeinträchtigt werden.